
Welcome to the latest edition of PHE’s Health Matters, a professional resource, which for this edition focuses on how the NHS Health Check is playing an important role in the prevention and early detection of cardiovascular disease (CVD) in England.
CVD is the number one cause of death globally, with an estimated 17.7 million people having died from CVD conditions in 2015, representing 31% of all global deaths. It is also a leading cause of disability and death in the UK, affecting around 7 million people and being responsible for 1 in 4 premature deaths in the UK, specifically 26% of all deaths in England in 2015.
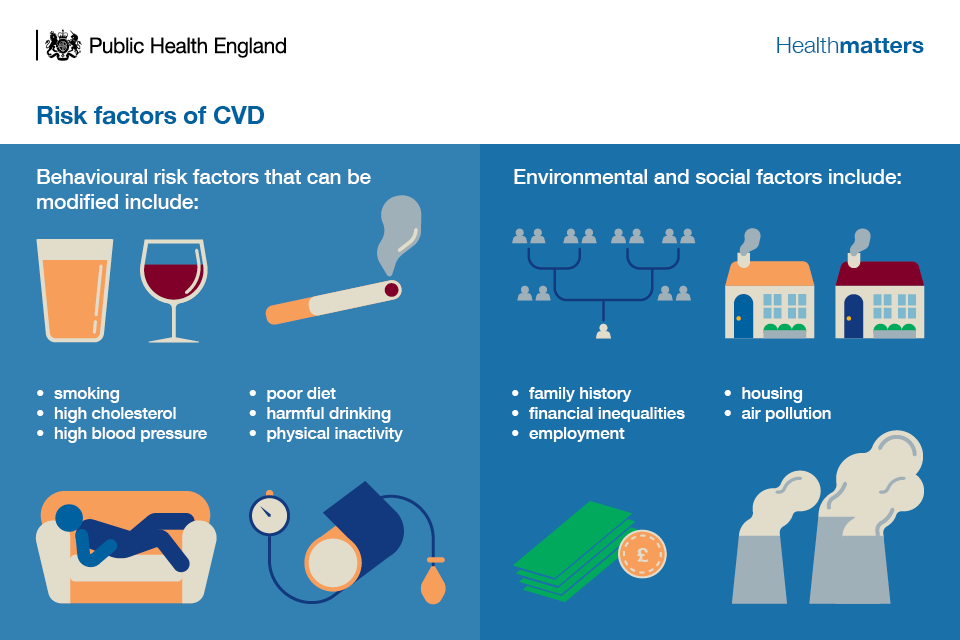
An estimated 50% to 80% of CVD cases are caused by modifiable and preventable risk factors, including:
- smoking
- obesity
- hypertension
- high cholesterol
- harmful drinking
- poor diet
- physical inactivity
These risk factors are greater in lower socioeconomic groups, making CVD one of the conditions most strongly associated with health inequalities. As a result, premature death rates from CVD in the most deprived 10% of the population are almost twice as high as rates in the least deprived 10%.
CVD also places a considerable strain on the NHS and wider society, accounting for an estimated £8.96 billion a year in NHS healthcare costs alone. With tighter budgets across the NHS and local government, it’s imperative that investment goes towards the most cost-effective CVD prevention interventions.
The burden of CVD on individuals, communities and the NHS is highly preventable through support for individual behaviour change, population measures such as tobacco control, and individual level interventions. However, in England, prevention is being limited by the diagnosis and treatment gap for major CVD risk conditions, including hypertension (high blood pressure) and atrial fibrillation (AF).
This edition of Health Matters focuses specifically on the role of the NHS Health Check in preventing and treating CVD. I believe that this programme is world-leading and arguably one of the largest prevention programmes of its type in the world, with almost 1.5 million people having the check every year.
By promoting healthy ageing and tackling the top 7 risk factors for early death and disability identified in the Global Burden of Disease study, the NHS Health Check also provides a cornerstone for the prevention of other diseases that share common risk factors for CVD such as dementia and some types of cancer.

Since April 2013, over 12.7 million people (82.5% of the expected eligible population) have been offered an NHS Health Check, and more importantly, 6.1 million people have received a check. Uptake has remained stable, with the national rate currently at 48.4%. However, this means that just over half of all people invited do not take up the offer.
Increasing uptake is crucial as the potential outcomes are significant. For example, for every 6 to 10 NHS Health Checks, 1 person is identified as being at high risk of CVD. Furthermore, research has shown that people who attend an NHS Health Check are more likely to be referred to lifestyle management services than those who do not attend.

To acknowledge the crucial role the NHS Health Check is playing in the prevention, early detection and management of non-communicable diseases (specifically CVD), PHE has recently published a stocktake and action plan on the programme. This document celebrates the achievements of the programme over the past several years but also importantly identifies 5 key priority areas for action. PHE will work with partners on these key actions over the coming 5 years to ensure that the programme achieves its full potential to support individuals and communities to reduce the burden of preventable disease, whilst also aiming to reduce the financial costs to our health and care system and society as a whole.
Read this edition of Health Matters to find out how NHS Health Check providers, NHS Commissioners, health and social care professionals, third sector charities and local authorities can contribute towards increasing uptake of the NHS Health Check. It includes a set of infographics and slides to support local commissioning and service delivery, as well as best practice case studies.
Visit the Health Matters area of GOV.UK to see the wide range of topics Health Matters has covered (other recent editions have looked at productive healthy ageing and musculoskeletal health, preventing infections and reducing AMR, alcohol and tobacco use, cervical screening, and child dental health) or sign up to receive the latest updates through our e-bulletin.
And if you found this blog helpful, please view other Health Matters blogs.
Health Matters
Health Matters is a resource for professionals which brings together the latest data and evidence, makes the case for effective public health interventions and highlights tools and resources that can facilitate local or national action. Visit the Health Matters area of GOV.UK or sign up to receive the latest updates through our e-bulletin. If you found this blog helpful, please view other Health Matters blogs.

6 comments
Comment by MARGARET R HOOK posted on
The use of trained pharmacy support staff should also be included - NOT only the pharmacist to increase the number of health checks available within local community pharmacies. When I trained to provide NHS Health Checks nurses and phlebotomists were invited to attend but only qualified pharmacists were. invited and considered eligible from my pharmacy team.
This is a huge oversight and misses the potential that could be realised. I have 4 members of my pharmacy team who are not pharmacists trained to motivate and support change in behaviour within the Support to Stop smoking scheme at my pharmacy - surely they should also be comissioned and offered training to provide NHS health checks.
Comment by MARGARET R HOOK posted on
The availability of free or fast track referrals to Weight loss support/ exercise programs/ alcohol reduction programs/ prescribing of statins are NOT available for all pharmacists to offer within the NHS Health Check consultation and it is important to be able to offer the same standard of support to people in every sector so the potential health improvement can be realised.
As more pharmacists are qualified as Independent prescribers unless there us a mechanism for them to prescribe within the NHS there will be limited data collection.
The ability for both Read and Write permission within the Summary Care record is also imperative unless the current Pharmoutcomes platform is recognised and links directly to medical records.
There would also need to be a new direct public information campaign about the difference between the basic summary care record and the real necessity of authorising a record with “additional information”.
While providing NHS Medicine Use Reviews for patients in my practice they are shocked that I cannot see their test results and when I explain and give examples of when more information about their heath could be needed they ask why it is not automatically available when they give permission to view or in emmergency such as A&E.
Comment by Robert Axford posted on
With 1.5 million having the check every year, why is by treating blood pressure and cholesterol only able to prevent a very small number of 250 to 500 people having major cardiavascular events every year ?
How does this compare to the total number of major cardiovascular events which occur each year?
Comment by Jamie Waterall posted on
Jamie Waterall, National Lead for Cardiovascular Disease Prevention at PHE, healthmatters@phe.gov.uk
This is a great question! These numbers were based on the additional people being treated with statins and antihypertensive treatment following the NHS Health Check. However, we know that the numbers are likely to be much greater when we consider all elements of the programme. Liverpool University have been commissioned to develop a new return on investment tool to allow us to consider the wider benefits of the NHS Health Check, which will give us a much more comprehensive picture.
Comment by Andrew Scott-Clark DPH Kent County Council posted on
Jamie
It is a real shame the NHS don't take NHS Health Checks seriously; the NHS Choices website, with regard to Stroke makes no mention of this programme and is consequently a missed opportunity to remind people to take up the offer when invited and get an NHS Health Check
Comment by Jamie Waterall posted on
Thank you Andrew for raising that important point. The NHS Choices website has a page dedicated solely to the NHS Health Check (https://www.nhs.uk/conditions/nhs-health-check/), which links through to further pages containing more information on what an NHS Health Check is, how to get one, and how to improve test results. However, I do see your point that not including a mention of the programme on the Stroke page could be a missed opportunity to direct people to the programme and remind them to take up the offer if they receive an invitation. We will flag your suggestion to extend the reference to the NHS Health Check programme on a wider number of the NHS Choices website pages.